
While we are proud to feature opinion pieces from our members and colleagues in the field, be advised that opinions and advertisements shared by NASW-CA do not necessarily reflect the views of the National Association of Social Workers, CA Chapter.
By Jason Bloome
Upcoming changes to asset limits will soon allow many aged and disabled residents in California to receive Medi-Cal benefits. Phase 1 begins in July 2022 when the current Medi-Cal asset limit: $2,000 for an individual and $3,000 for a couple will increase to $130,000 for a single person, $195,000 for a couple and $65,000 for each additional family member. Phase 2, beginning no sooner than January 2024, will eliminate the asset test entirely. The Department of Health Care Services will work together with the County Welfare Directors Association of California, consumer groups and county agencies to implement the Medi-Cal asset test changes.
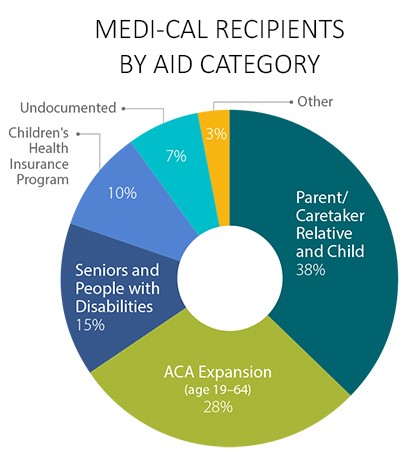
The Medi-Cal program was created by the California Medical Assistance Program in 1965 as a welfare program along with Head Start, Jobs Corp and the Food Stamp Act. Almost one is three (approximately 15 million) Californians are on Medi-Cal and, of these, approximately 15% (2 million) are aged and disabled. The program has vastly expanded over 60 years and many aged and disabled rely on Medi-Cal to pay for pricey medicines, in-home care, nursing home expenses and other costs not covered by Medicare.
The current Medi-Cal asset limit, which has not changed since 1989, is far below the low-income standards for many individuals in California who are defined by Covered California, the state’s health insurance marketplace, as receiving less than $47,520 per year. The asset test changes will allow many more aged and disabled individuals to receive Medi-Cal benefits and is expected to increase Medi-Cal access to 18,000 new beneficiaries and improve access to Medi-Cal benefits for approximately 2 million current Medi-Cal recipients.
The new Medi-Cal asset limits (and eventual elimination) will enable low-income aged and disabled individuals in California to develop a financial safety net (e.g., save money for rent, auto and house repairs, financial emergencies, etc.) without becoming impoverished to receive Medi-Cal.
The asset test changes will bring parity to Medi-Cal eligibility standards used for young recipients: the Modified Adjusted Gross Income (MAGI) with no asset limit and non-MAGI recipients (the aged and disabled) that have asset limitations through the Aged and Disabled Federal Poverty Level (A & D FPL). The qualifying standards for A & D FPL and MAGI will become the same and prevent the loss of Medi-Cal for young Medi-Cal recipients who age into Medicare (when reaching 65 or due to a disability).
The new changes will impact Medi-Cal programs that serve the aged and disabled: e.g., nursing home residents on long term support and services, Medicaid Waiver programs and Home and Community Home Based Services (HCBS). Increasing Medi-Cal access to HCBS programs with a limited cap on enrollment (e.g., the Assisted Living Waiver) will inevitably increase program waitlists.
Current individuals who receive Medi-Cal through the Social Security Supplemental Income (SSI) program will not be affected by the new Medi-Cal asset changes, but individuals who choose to retain assets and qualify for Medi-Cal based on income may no longer qualify for SSI benefits.
The 2022-2023 California fiscal budget allocates $394 million to cover the expected increase of Medi-Cal enrollment due to the asset test changes.
Jason Bloome is owner of Connections Care Home Consultants an information and referral agency for care homes for the elderly in Southern California
Sources:
















