
By Jason Bloome
NASW-CA News Contributor
Nursing homes in California have been hard hit by COVID-19 with more than 2,184 resident deaths due to the virus. Geriatricians and patient advocates have been pressuring the state to protect nursing home staff and residents by increased testing and isolation of infected residents. A lack of compliance, enforcement and arbitrary state guidelines for testing perpetuate nursing homes as settings where residents continue to be at high risk of contracting and dying from the virus.
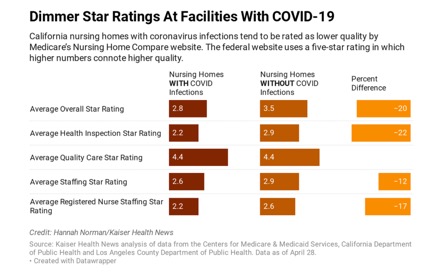
In mid-April the state mandated all nursing homes test their residents and staff, but the result was ineffective since many nursing homes still do not have comprehensive testing protocols. Homes that did report COVID-19 infections frequently had lower star ratings from Medicare Compare.
On May 22, 2020, the California Department of Public Health issued new specific surveillance and testing protocols which, in part, require all homes:
- Test 25% of their staff weekly ensuring 100% of their staff are tested each month with the frequency of testing to vary as determined by local county public health agencies depending on the spread of the virus in the community.
- Require in facilities where one or more residents test positive for COVID-19 the testing 100% of their residents every seven days for two weeks until there are no reported cases.
- Place residents, depending on their test results, in three separate cohorts:
A. Residents who test positive
B. Residents who test negative with known exposure within 14 days.
C. Residents who test negative with no known exposure within 14 day. - Place residents who test positive in separate parts of the facility with dedicated health care staff who do not provide care for members in other cohort groups.
- Establish a plan for testing which includes tracking and informing staff, residents and families of testing results.
- Establish a plan to account for staff shortages if positive staff are excluded from working.
- Allow staff who test positive to work if they wear masks and only care for COVID-19 positive residents.
- Require all residents be tested prior to admission or readmission and, in cases where the testing is not done by the hospital or other healthcare facility, test and quarantine the incoming resident in a private room for 14 days.
- Establish a relationship with laboratories to process the COVID-19 tests.
- Establish a procedure for residents and staff who refuse to be tested in homes where they are positive cases (e.g. a symptomatic resident refusing to be tested should be treated as positive).
Despite the new directives, many patient and healthcare advocacy groups are concerned the new state guidelines will continue to be ineffective by merely shifting responsibility for testing onto counties and nursing homes. The result: a patchwork of uncoordinated plans for testing, contracting with testing facilities and uncertainty as to who reimburse nursing homes for testing and PPE.
Concerned about the lack of statewide instruction, many counties plagued by COVID-19 have enacted additional nursing home measures. In Los Angeles, the largest county in California with the highest number (1000+) of COVID-19 related nursing home deaths, the Board of Supervisors unanimously approved the appointment by July 1st of a new inspector general to oversee nursing homes.
The inspector general is expected to address the failures that many see in the county’s slow response to COVID-19 in nursing homes where deaths related to the virus account for ½ of all COVID-19 fatalities in the county.
According to Supervisor Mark Ridley-Thomas, the new nursing home inspector general’s role will be to “provide an extensive review of the county’s capacity to regulate these facilities, recommend structural and operational changes, and outline a plan for ensuring adequate and sustainable oversight”.
The Board of Supervisors also approved the development of a new dashboard on the county’s website with information about each nursing home’s total COVID-19 cases, frequency of testing, number of deaths broken out by residents and staff members, and the status of the home’s outbreak mitigation plan.
Jason Bloome is owner of Connections – Care Home Consultants, an information and referral agency to care homes in Southern California. More information at carehomefinders.com.
Sources:
https://www.cdph.ca.gov/Programs/CHCQ/LCP/Pages/AFL-20-53.aspx















